Key Takeaways
- Despite widespread access to company wellness programs, participation often remains low due to unclear communication and a lack of relevance.
- Employees are more likely to engage when wellness benefits are explained in simple, personalized messages that clearly outline the value and next steps.
- Using multiple communication channels, visual formats, and continuous reminders helps keep wellness programs visible and accessible.
- Data-driven strategies such as A/B testing and engagement tracking enable organizations to refine messaging and increase enrollment in employee wellness initiatives.
Despite the growing focus on employee well-being, participation in wellness initiatives remains a challenge. According to SHRM’s Employee Benefits Survey, only 39% of employers report offering wellness programs with dedicated resources which is a decline from previous years. As organizations continue to invest in employee wellness, ensuring those programs are actively used has become more important than ever.
That gap between offering and action often stems from communication failures. Workplace benefits are announced once, buried in HR-speak, or delivered through channels employees rarely check.
In the sections that follow, we explore why employees so frequently tune out benefits messaging, how to craft benefit communications that truly resonate, and how to deploy strategic nudges and measurement tactics to increase enrollment and engagement rates in wellness programs.
Why Employees Tune Out Company Wellness Programs
Employees aren’t ignoring wellness benefits because they don’t care about their health. They tune out because the messaging often makes it hard to connect the dots.
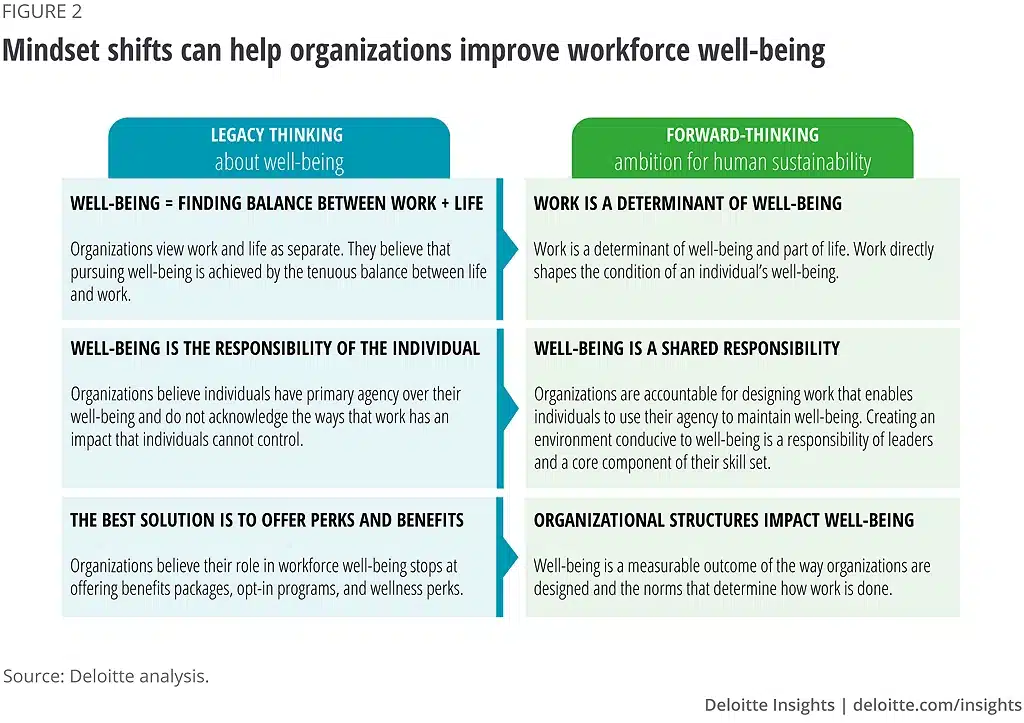
Many organizations still approach employee well-being as a set of optional workplace benefits rather than a shared responsibility embedded in workplace design. The shift from “perk-based well-being” to “organizational well-being” is increasingly emphasized in workplace research. Yet, even when organizations invest in wellness initiatives, participation often falls short because of how those benefits are communicated to employees.
1. Overwhelming, One-Time, or Poorly Timed Communication
Many organizations rely heavily on annual enrollment announcements that include dense emails, long PDFs, and multiple benefits rolled into a single message during an already busy period.
The result?
Employees can’t process that much information at once. Details are forgotten quickly. The timing rarely matches when someone actually needs the benefit.
For example, a caregiver juggling family responsibilities may not pay attention to mental health support in January, but they might desperately need it in April. When communication is limited to one season, relevance is often lost.
2. Too Complex or Filled With HR Jargon
Terms like “preventive care utilization,” “HSA-eligible services,” or “biometric screening incentives” may be accurate, but they rarely connect. In fact, 7 out of 10 employees say they don’t fully understand the workplace benefits designed to protect their health, finances, and families.
Employees are silently asking one question:
“What does this mean for me right now?”
If they have to decode the language before understanding the value, most employees simply move on without exploring the benefit further.
3. Not Personalized to Real Employee Needs
A single, generic message rarely speaks to everyone. When communication feels broad and impersonal, employees assume the benefit isn’t meant for them. Many organizations also discover that simply offering perks isn’t enough to drive participation. Strategies focused on encouraging participation in wellness programs can help organizations move beyond passive benefits and create more meaningful engagement. For example:
- Gen Z employees may value mental health apps and flexibility
- Parents may prioritize family coverage and stress management
- Remote workers may want virtual fitness or digital health tools
- Frontline teams may need on-site resources
4. Sent Through the Wrong Channels
Even a well-written message fails if it never reaches the right audience. For example,
frontline workers may not check email regularly, remote employees might skip intranet updates, and desk-based teams may overlook app notifications.
When communication channels don’t match how employees actually work, the message tends to disappear within the company wellness program communications.
How to Communicate Your Employee Wellness Program So Employees Actually Enroll
So how do you turn wellness communication from background noise into a clear call to action?
It starts with structure.
Employees pay attention to employee wellness messages when they are simple, relevant, and easy to act on. A strong communication strategy removes confusion and reduces friction. The goal is to make the next step obvious.
Employees consistently say they want clearer communication, improved access, and more relevant workplace benefits, reinforcing the importance of structured messaging.

So, what are some steps that can be taken to ensure that the benefits are conveyed effectively?
1. Use the “Why → What → How → Impact” Framework
A simple message structure makes benefits easier to understand and act on.
- WHY it matters
Start by connecting the benefit to a real challenge employees face. When employees recognize the problem, they’re more likely to keep reading.
Example: “Feeling stretched between work and family responsibilities?”
- WHAT the benefit will provide
Describe the offering in one clear, jargon-free sentence.
Example: “Our wellness platform offers confidential mental health sessions and stress management resources at no cost.”
- HOW to enroll
Give one direct action step with a single link or instruction. Avoid multiple buttons or long explanations. The easier the action, the higher the enrollment.
Example: “Click here to activate your account in under two minutes.”
- IMPACT it will have
When employees understand both the practical steps and the personal benefit, there is more motivation to join company wellness programs.
Example: “Feel more supported, reduce stress, and access help when you need it.”
2. Use Multiple Channels to Reach Everyone
Even the clearest message won’t work if it doesn’t reach the right people. Different employee groups consume information differently. Effective communication meets them where they already are:
- Email for short, scannable updates with one clear CTA
- SMS or push notifications for timely reminders
- Intranet or benefits portals for FAQs and step-by-step guides
- On-site posters or digital signage for offline teams
- Manager talking points to reinforce trust and answer questions
- Short videos to simplify complex benefits
A multi-channel approach ensures that communication about your employee wellness program doesn’t rely on a single touchpoint.
3.Use Simple, Visual Formats
Employees are busy. Long paragraphs and policy-heavy documents don’t get read.
Instead, use:
- Infographics to summarize benefits quickly
- Comparison tables to clarify options
- Short step-by-step visuals for enrollment
- Real-life examples that show how the benefit fits into everyday situations
Visual clarity reduces hesitation. And when hesitation decreases, enrollment increases.
4. Communicate Continuously, Not Just During Enrollment Season
One announcement is rarely enough. Employees need multiple touchpoints before taking action. A simple rhythm works well:
- Early teaser (“Coming next month: expanded wellness support.”)
- Launch announcement
- Mid-cycle reminder
- Final deadline nudge
When communication is ongoing rather than annual, your company wellness programs stay visible and, in turn, drive participation.
Turning Awareness Into Action: Smart Enrollment Nudges That Work
Remove friction from the first step: Direct enrollment links and simplified steps make it easier for employees to understand and engage with workplace benefits.
1. Use Well-Timed Nudges
The more effort enrollment requires, the less likely employees are to complete it. Instead of sending employees to a homepage and asking them to “find the wellness section,” provide a direct enrollment link. Add a short explanation of what to expect and include a clear time estimate, such as “Takes less than 3 minutes.”
When the path is obvious and simple, action feels manageable.
2. Personalize Reminders
Send reminders after major work cycles or deadlines. Nudge employees before key well-being initiatives or challenges begin. For example, someone who joined a step challenge last quarter may be more likely to enroll in a new fitness initiative. Relevance increases response.
3. Leverage Social Proof
Share participation stories or simple engagement stats to create positive peer influence and encourage others to join. For example, “Over 60% of our team has already activated their wellness account.”
5. Offer Small Incentives
Sometimes the hardest part is getting started. Early-enrollment rewards, badges, or point-based recognition can motivate employees to take the first step. Once they experience the benefit, continued engagement becomes more likely.
A/B Testing Messages and Measuring Enrollment Lift
A/B testing allows organizations to compare two versions of a message, such as different subject lines, calls-to-action, or send times, to see which one drives more engagement and enrollment.
Instead of relying on assumptions, HR teams can use data to identify what actually resonates with employees.
Track metrics such as:
- Open rates
- Click-through rates
- Enrollment conversions
Most importantly, measure enrollment lift, the increase in sign-ups that can be directly tied to a specific communication campaign.
Small adjustments in wording or timing can lead to meaningful increases in participation. Over time, testing and refining messages creates a continuous improvement cycle, thereby strengthening engagement across your employee benefits initiatives.
Build a Communication Engine That Drives Company Wellness Enrollment
Clear communication transforms workplace benefits from overlooked offerings into meaningful resources that employees actively use to improve their health and well-being. But to sustain participation, organizations need a connected strategy.
CoreHealth NOW brings well-being tools, insights, and engagement strategies together into one all-in-one platform designed to improve well-being, participation, and ROI.
Explore how CoreHealth can help you increase enrollment and engagement across your workforce.